Athletic Pubalgia (Sports Hernia)
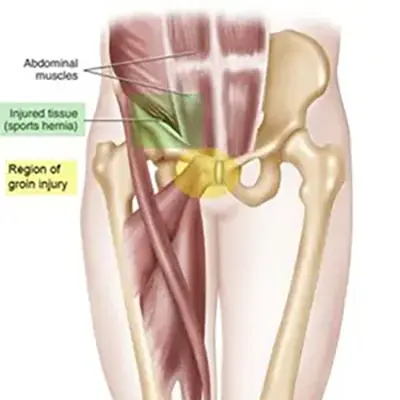
What is Athletic Pubalgia?
Athletic pubalgia, also known as sports-hernia or Gilmore’s groin, is a condition that causes chronic pain in the groin and pelvic region due to damage or strain of soft tissues. It is most commonly seen in athletes who perform vigorous movements involving twisting, sudden direction changes, or repetitive stress. While not a true hernia, athletic pubalgia can sometimes contribute to hernia development.
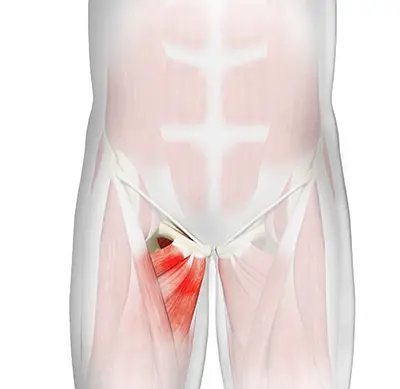
Causes of Athletic Pubalgia
The condition is typically caused by intense twisting or repetitive motions, often seen in sports such as hockey, soccer, football, tennis, and skiing. Men are at higher risk because a narrower pelvis may provide less stability in the groin area. Other conditions that can cause similar groin pain include:
- Nerve compression
- Genitourinary issues
- Previous injuries
- Rectus-adductor syndrome
Dr. Benjamin Domb and his team evaluate each patient to differentiate athletic pubalgia from these other conditions.

Symptoms of Athletic Pubalgia
Symptoms may vary but commonly include:
- Pain on one side of the groin or lower abdomen during activity
- Chronic pain that limits return to sports
- Sharp pain at the time of injury that may later subside but worsen with activity
- Tenderness in the groin, upper thigh, or lower abdomen
- Bruising or swelling
- Groin stiffness
- Muscle weakness that can sometimes lead to a true hernia
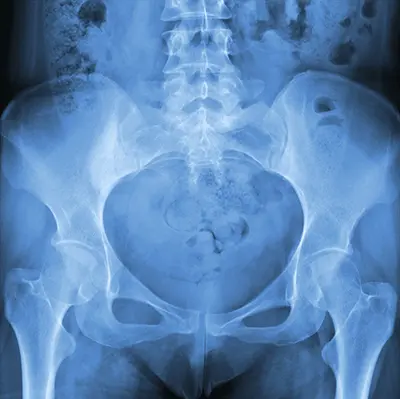
Diagnosis of Athletic Pubalgia
Diagnosing athletic pubalgia can be challenging because groin pain may have multiple causes. Dr. Domb and his team use a combination of medical history, physical examination, and imaging studies to confirm the diagnosis:
- MRI: Provides detailed images of soft tissues, muscles, tendons, and ligaments; considered the most definitive test for athletic pubalgia
- CT Scan: Gives cross-sectional images of the pelvis and groin
- X-rays: Helps rule out fractures
- Ultrasound: Assesses surrounding soft tissues and excludes inguinal hernia
- Bone Scan: Detects bone injury

Conservative treatments
For most patients, non-surgical options are tried first:
- Anti-inflammatory medications (NSAIDs) to reduce pain and swelling
- Rest and activity modification for 4–6 weeks
- Ice therapy to relieve pain and inflammation
- Injections, such as corticosteroids or platelet-rich plasma (PRP), to promote healing
- Physical therapy to strengthen the groin and abdominal muscles
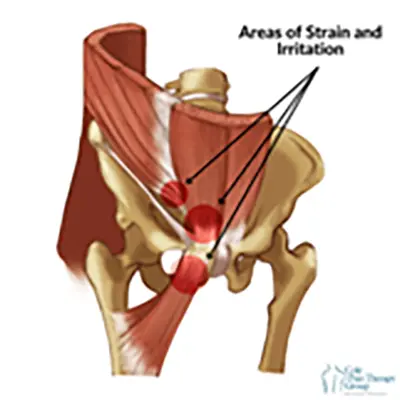
Surgical treatment
If conservative treatment is ineffective or the injury is severe, surgery may be recommended:
- Open surgery: A larger incision allows full access to repair the damaged tissues
- Laparoscopic surgery: Minimally invasive procedure using a small camera and specialized instruments to repair the tissues
- Inguinal neurectomy: If chronic pain is caused by a damaged inguinal nerve, the nerve may be surgically removed
Recovery after surgery generally takes 6-8 weeks. In cases of persistent pain, a secondary procedure called an adductor tenotomy may be performed. This involves lengthening the tendons of the inner thigh muscles to relieve tension and improve function.
