Shoulder
Shoulder
Shoulder Anatomy
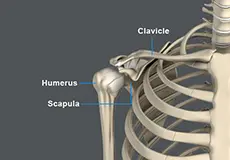
The shoulder is the most flexible joint in the body that enables a wide range of movements including forward flexion, abduction, adduction, external rotation, internal rotation, and 360-degree circumduction. Thus, the shoulder joint is considered the most insecure joint of the body, but the support of ligaments, muscles, and tendons function to provide the required stability.
