Knee
Knee Anatomy
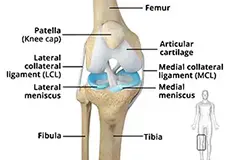
The knee is a complex joint made up of different structures - bones, tendons, ligaments, and muscles. They all work together to maintain the knee's normal function and provide stability to the knee during movement.

The knee is a complex joint made up of different structures - bones, tendons, ligaments, and muscles. They all work together to maintain the knee's normal function and provide stability to the knee during movement.
999 E Touhy, Suite 450
Des Plaines, IL 60018
9615 Keilman St
St John, IN 46373
270 W Loop Rd
Wheaton, IL 60189
111 N. Wabash Ave. Suite 1919
Chicago, IL. 60602
