Hip
-
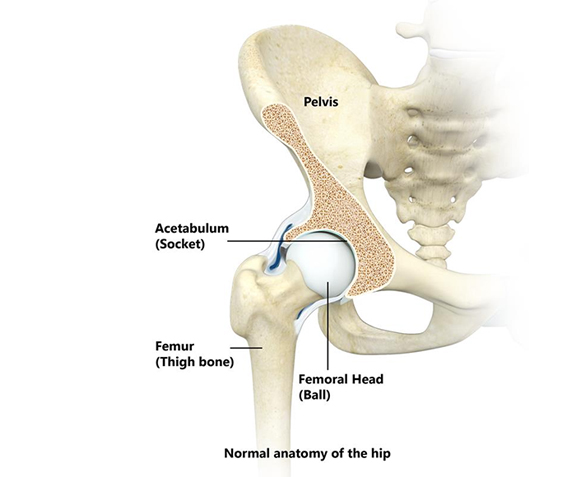
Hip Anatomy
To gain a deeper understanding of how the hip joint functions and its important structures, click here to learn more about hip anatomy.
-
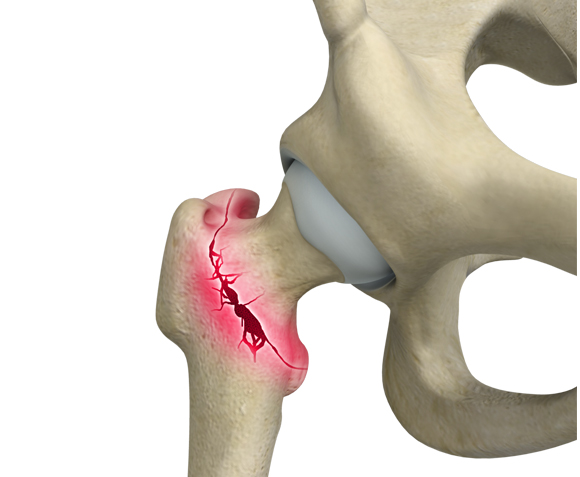
Hip Injuries & Conditions
Click here to learn more about common hip conditions, including their causes, symptoms, and how they affect the joint.
-
Non-Surgical Treatments
Click here to learn more about non-surgical treatments for hip conditions, including physical therapy, lifestyle modifications, and other conservative approaches.
-
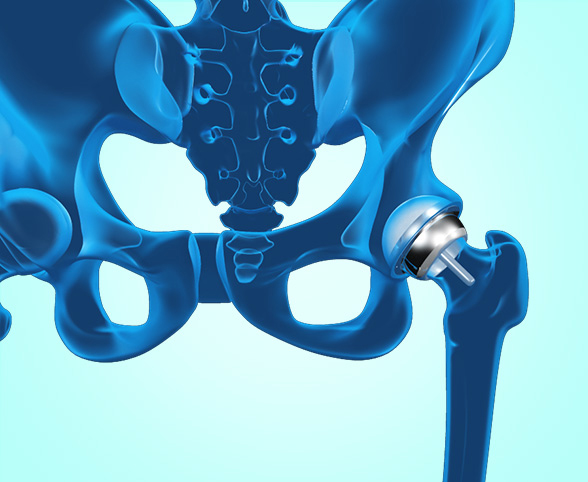
Surgical Treatment Options Offered by Dr. Domb
Click here to learn more about surgical treatment options for hip conditions, including procedures designed to restore function and relieve pain.